Saving unborn babies from brain damage with new MRI scanning techniques
New MRI scanning techniques, developed with over £270,740 of funding across two grants from Action Medical Research, are helping to save unborn babies who are at risk of brain damage and other life-threatening or life-changing conditions.
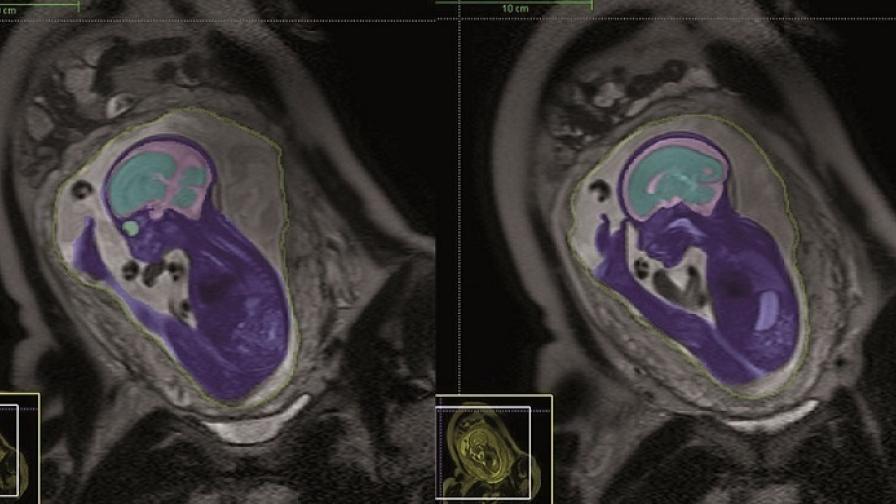
Accurate 3D images can now be captured even when an unborn baby or the mother does not stay perfectly still and the process, which used to take 12 hours, now takes just 30 minutes.
This helps doctors diagnose brain disorders that can lead to problems such as cerebral palsy or autism. Treatment decisions can be made more quickly, saving babies’ lives. In one case, an unborn baby with a swollen vein deep inside the brain was delivered early following MRI scanning and taken straight for surgery. If he had been left just 24 hours longer, he would have been severely brain damaged or died.
Other organs, such as the heart and kidneys, can also be studied using this technique, which was developed by Professor Mary Rutherford and her team at Hammersmith Hospital, London (now St Thomas’s Hospital, London).
The Action funding also allowed Professor Rutherford to develop a special mapping technique which helps to identify unborn babies who are at risk of brain damage caused by reduced blood flow and oxygen to the brain. This scan can be completed in the time a mother can hold her breath – 23 seconds – and is especially helpful for identical twins who share a placenta, or whose mother is severely ill.
With MRI scanning being requested more frequently, these new techniques are helping to reduce the suffering and save the lives of hundreds more vulnerable unborn babies in the UK and across the world.

