Barnaby's story
Epilepsy
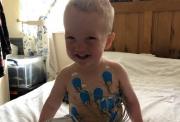
On his worst days, three-year-old Barnaby has had as many as 100 seizures. Keeping their young son safe and well is a constant challenge for parents Charlotte and Kieran.
Lilly-May’s: Rasmussen’s encephalitis
Lilly-May underwent life-changing brain surgery due to the rare condition Rasmussen's encephalitis
Luke's story: brain tumour
Living with a brain tumour through the COVID-19 pandemic
Mollie: Rett syndrome
Mollie has Rett syndrome, a rare and severe neurological condition that primarily affects girls and leads to severe physical and learning disabilities.
Tom: Wolfram syndrome
16-year-old Tom is living with the rare and progressive neurodegenerative disorder, Wolfram syndrome.
Barnaby: epilepsy
On his worst days, Barnaby has had as many as 100 seizures. Keeping their young son safe and well is a constant challenge for parents Charlotte and Kieran.
Digby’s story: Duchenne muscular dystrophy
Ten-year-old Digby is living with the rare genetic condition, Duchenne muscular dystrophy.
Elsie's story: premature birth
Elsie was born extremely prematurely at 23 weeks and 5 days and weighed just 600 grams. She developed serious complications and spent a total of 211 days in the NICU.
Oscar: neurofibromatosis type 2
Oscar has neurofibromatosis type 2, a rare condition that causes multiple slow-growing tumours in different parts of the nervous system, including around the brain and spine.
Poppy: Frame Running
Poppy has a rare neuromuscular condition which has left her with paralysis and weakness in her upper body and core. She has benefited from taking part in Frame Running, a sport developed for young people with limited mobility.
Tora: neurofibromatosis type 1
Tora has neurofibromatosis type 1 (NF1), a rare condition that causes tumours to grow along nerves. This can cause a wide range of symptoms and treatment options are very limited.
Eva: rare liver disease
Eva has progressive familial intrahepatic cholestasis type 3 (PFIC3), a very rare inherited liver disease that over time causes severe damage.
Mylo: congenital CMV
At three months old Mylo was diagnosed with congenital cytomegalovirus (CMV) a common and usually harmless virus but it can sometimes cause serious disabilities in babies who contract it during pregnancy.
George: lung surfactant deficiency
George was diagnosed with lung surfactant deficiency (ABCA3 deficiency) as a small baby.
Emmy: Vici syndrome
Emmy has Vici syndrome, a very rare and life-limiting genetic disorder. Sadly, there is currently no cure or effective treatment and most affected children lose their lives at a very young age.
Evan: medulloblastoma
Evan was diagnosed with medulloblastoma when he was 15 months old.
Naomi: epidermolysis bullosa simplex
Naomi has a rare, inherited skin disorder called epidermolysis bullosa simplex (EBS) which means her skin is fragile and blisters easily in places where it is rubbed or scratched.
Henry: hypertrophic cardiomyopathy
Henry was born with a genetic heart disease called hypertrophic cardiomyopathy (HCM).
Robi: CDA-1 anaemia
Thirteen year old Robi has a rare, inherited type of anaemia called congenital dyserythropoietic anaemia type 1 (CDA-1).
Paddy: KCNT1-related epilepsy
Paddy has a rare disease which has no cure and has left him severely disabled. Since he was a tiny baby, he has suffered thousands of seizures. Most devastatingly of all, children with this condition often don’t live into double figures.
Rosie and May: Long COVID
Siblings Rosie and May have been severely impacted by the effects of COVID-19 and continue to suffer, both physically and mentally, with the long-term effects of the virus – also known as long COVID.
James and Samuel: X-linked lymphoproliferative disease (XLP)
Brothers James and Samuel both have X-linked lymphoproliferative disease (XLP) – an extremely rare and life-limiting, inherited disease. The boys both underwent bone marrow transplants and youngest Samuel is doing well. Sadly, James passed away in August 2023.
Fletcher: Extremely premature birth
Fletcher was born extremely prematurely at 24 weeks and 4 days, weighing just 705 grams. He endured 15 weeks of treatment in the Neonatal Intensive Care Unit (NICU) due to serious complications including sepsis, E.coli infection, pneumonia and necrotising enterocolitis (NEC).
Finley: Diamond-Blackfan Anaemia (DBA)
Finley has Diamond-Blackfan anaemia, a very rare condition where the bone marrow fails to produce enough red blood cells. There is currently no cure, so children like Finley rely on long-term treatment.
Beatrice: NMDAR-antibody encephalitis
Aged just eight and previously healthy, Beatrice endured the terrifying effects of autoimmune encephalitis – a rare type of brain inflammation, which caused her to lose the ability to walk or speak for several months.
Danny: Hunter syndrome
Danny’s family are painfully aware that time with their youngest son will be cruelly cut short by Hunter syndrome, a rare disease with no cure and limited treatment options.
Sophia: spinal muscular atrophy
Sophia was diagnosed with spinal muscular atrophy type 1 just before her first birthday. This rare disease causes loss of movement and muscle wasting.
Wilfred: premature birth, NEC and cerebral palsy
Little Wilfred's sunny nature is especially precious to his parents, who feared they would lose him to dangerous bowel disease NEC after he was born prematurely.
Ian: Frame Running
With cerebral palsy affecting one side of his body, Ian faces difficulties with his muscle strength, stiffness, co-ordination and balance.
Edward: Treating severe dystonia
Edward developed debilitating dystonia when he was 16 months old. It caused him to suffer uncontrollable, painful spasms – and his case was one of the worst doctors had ever seen
Matilda: Niemann-Pick disease type C
Matilda has the very rare neurodegenerative disease Niemann-Pick disease type C (NPC).
Sophia: cystic fibrosis
Little Sophia who has cystic fibrosis lives with a daily treatment regime to help protect her lungs.
Alice: cerebral palsy
Alice, who was born prematurely at 32 weeks, faces a lifetime of challenges because her ability to move is severely impaired by cerebral palsy.
Millie and Scarlett: premature birth and NEC
Millie, who was born at just 28 weeks, is a loving child with a startlingly mature awareness of her twin sister Scarlett, who tragically died aged just one month.
Elijah: necrotising enterocolitis (NEC)
Elijah was born extremely prematurely at 25 weeks and three days, weighing just 823g and, sadly, lived for just 37 days.
Felix: neuroblastoma
Felix was diagnosed with high risk, stage four neuroblastoma aged just four and tragically lost his life after two years of gruelling treatment.
Tom: cerebral palsy
Tom was diagnosed with quadriplegic cerebral palsy before his first birthday and discovering that their baby son would face a lifetime of disability was heartbreaking for Maria and husband Terry
Jacob: premature birth
The determined cries of her one-year-old son mean the world to Rachel and her husband Carl, since little fighter Jacob was born at just 30 weeks after Rachel developed the serious pregnancy complication pre-eclampsia.
Georgia: Crohn's disease
Georgia was a healthy baby but at around 12 months old, her stools became looser and she developed a severe rash. After becoming very unwell with a high temperature she was admitted to hospital.
Emma: premature birth
After emergency tests in hospital, Inge was given the shocking news that she had a life-threatening pregnancy complication. Baby Emma was born 12 weeks early, weighing just 1lb 13oz and measuring less than 30cm long.
Robbie: cleft palate
Shortly after his birth, Robbie was diagnosed with a condition called Pierre Robin Sequence. He had difficulty feeding and breathing due to a cleft soft palate and a small, receding lower jaw.
Aiden: neonatal encephalopathy (NE)
Aiden suffered from a shortage of oxygen at birth and was whisked away to the intensive care unit where the team began to reduce his body temperature to protect him from brain damage.
Freya: premature birth
Freya was born three months early weighing just 2lbs 4oz after Steph developed a life-threatening pregnancy complication.
Sophie: epilepsy
Recalling the time when her daughter Sophie’s seizures first began, mum Anne says: “Sophie first noticed something unusual happening when she was cross country running aged 11.
Noah: Landau Kleffner syndrome
When little Noah was diagnosed with the rare disease Landau Kleffner syndrome, doctors told his parents Madeka and Ryan, ‘Don’t look it up because it will really scare you’.
Joey: brain cancer
When Joey was just four years old, his parents Darren and Kathryn faced the terrible news that their little boy had a brain tumour.
Toby, Corey and Izzy: Juvenile Batten disease
Discovering that three of their children have the devastating, rare condition juvenile Batten disease has, says mum Dee, left the family feeling numb.
Jack: premature birth and NEC
Born extremely prematurely, Jack has made remarkable progress. He is now a happy pre-schooler but, due to his early birth, faces potential health and developmental issues as he grows up.
Sophie: birth asphyxia
Natasha wasn’t able to hold her daughter until she was five days old, so cuddles are even more precious now. Baby Sophie was born blue and totally unresponsive due to complications which led to her being starved of oxygen.
Jessica: Hypoplastic Left Heart Syndrome
Jessica had a heart problem called hypoplastic left heart syndrome (HLHS) which affects one baby in 5,000. The left side of her heart was much smaller than usual, and could not pump enough blood to the body.
Lucas and Oscar: premature birth
Twins Lucas and Oscar are the best of friends even though they are very different. Their mum, Meg, feels blessed that both boys are happy and healthy, as they were born very prematurely, at just 31 weeks.
Samuel: premature birth
Jo was admitted to hospital for emergency surgery 29 weeks into her pregnancy and nobody knew what the outcome would be. Thankfully, she and husband are now the proud parents of Samuel, who survived being born at just 30 weeks.
Emily: premature birth & pre-eclampsia
Emily was born at just 34 weeks after her mum, Tracy, developed pre-eclampsia – a condition which affects up to eight per cent of pregnant women worldwide and is a leading cause of death and illness in both mothers and babies.
Daisy: premature birth
Daisy, who was born 13 weeks early, is now at school and has recently started gymnastics - and has become a big sister to baby Poppy, who also arrived early, five weeks before her due date. But Daisy's earliest days were a roller coaster of ups and downs.
Emma: congenital hypothyroidism
Emma’s arrival was problem-free but, when she was just nine days old, mum Nicky received a call from Lewisham Hospital Paediatric Team asking to see her daughter as a matter of urgency.
Iris and Tom: Pre-eclampsia & premature birth
For Maria and husband Terry it is an especially precious memory leaving hospital with two babies, since the serious pregnancy complication pre-eclampsia resulted in the twins being born two months early by emergency caesarean section.
Tom: Duchenne
Tom was diagnosed with Duchenne when he was four, but his parents were concerned about him from his earliest days.